Brazil is suffering from diseases caused by arboviruses, which are viruses transmitted by arthropods, such as mosquitoes. In case there was any doubt: we are indeed experiencing a Dengue epidemic, with an incidence about twice as high as that observed last year ( Weekly Arbovirus Report ). Other known arboviruses are Zika, Chikungunya, and Yellow Fever. But today we are going to talk about a virus discovered over 60 years ago, which causes disease in humans, mainly in the Amazon region. Thus, this is yet another virus that causes a disease that is part of the so-called “neglected tropical diseases”.
This is Oropouche fever, have you heard of it?
If you are from the northern region of Brazil, probably yes.
This latest outbreak, which is still ongoing, has already recorded more than 2,000 cases. As of March 6, the Pan American Health Organization (PAHO) had recorded 1,821 cases in Amazonas, 172 in Rondônia, 51 in Acre, and 12 in Roraima. The city of Manaus reported 829 cases confirmed by laboratory criteria as of March 2, 2024, and the death of a young woman who was infected with the Oropouche virus (OROV) and who also had COVID-19.
It is worth noting here that the emergence and reemergence of arboviruses is not trivial. Therefore, it serves as a warning about human interventions in the environment. As well as carelessness, lack of diagnosis, and negligence in understanding the real impact of many tropical diseases.
Between the beginning of January 2024 and April 9, 2024, 3,324 cases were identified. Divided between the states of the North region Amazonas (2,575), Rondônia (592), Acre (110), Roraima (18), Pará (29). An increase of 400% compared to 2023.
Oropouche Fever, what virus is this?
To understand the composition of a virus. It may be important to understand that it is divided into two parts: the envelope and the viral particle. In Oropouche, the envelope is lipoprotein. That is, the outside of the virus is a layer composed of fat (“lipo”) and proteins (“protein”).
The viral particle, its genetic material, is single-stranded RNA. Divided into three fragments: a small one (S), a medium one (M), and a longer one (L). The particle has glycoproteins on its surface, and an enzyme responsible for viral replication, an RNA-dependent RNA polymerase (RdRp). In other words, an enzyme is capable of making an RNA molecule using another RNA molecule as a template (Figure 1).
Oropouche Fever: Diseases in humans and animals
This virus belongs to the family Peribunyaviridae, along with other viruses that cause diseases in humans and animals. It was discovered in 1955 in a febrile patient in the village of Vega de Oropouche in Trinidad and Tobago. Since then, outbreaks have been identified in countries such as Brazil, Peru, Colombia, French Guiana, and Panama. More than 500,000 cases of the disease have been reported previously.
 Figure 1. Oropouche fever: viral particle and common symptoms. S = small fragment; M = medium fragment; L = long fragment; RdRp = RNA-dependent RNA polymerase.
Figure 1. Oropouche fever: viral particle and common symptoms. S = small fragment; M = medium fragment; L = long fragment; RdRp = RNA-dependent RNA polymerase.
That’s a pretty high number for a little-known infectious disease, don’t you think? And it doesn’t stop there…
Immune surveillance studies, which assess the presence of antibodies in people’s blood indicating that there has been a previous infection, indicate that many other cases may have gone unnoticed, without diagnosis, over the years. For example, some regions in the Amazon indicate a high seroprevalence (proportion of people in a population who have specific antibodies in their blood at a given time), with up to 50% of people having antibodies to Oropouche, indicating a response to previous exposure to the infectious agent.
Characteristics of Oropouche Fever
The disease, known as Oropouche fever, has an incubation period of 4 to 8 days. That is, from transmission to the appearance of symptoms. The most common symptoms are a fever of around 39°C, muscle pain (myalgia), joint pain (arthralgia), chills, nausea, vomiting, and dizziness.
Additionally, some people may experience a condition called photophobia, which is when the eyes become very sensitive to light, causing discomfort. However, pain in the eye area, anorexia, and weakness may also occur.
Symptoms last around 7 days, and approximately 60% of people may experience a relapse (reappearance of symptoms after a period of remission or recovery) around two weeks later. Which may return more severely. That is, symptoms may reappear as a consequence of this infection and do not constitute a new infection.
Less frequent symptoms
Less frequent symptoms described in the literature include hemorrhagic phenomena such as bleeding gums and the appearance of red spots on the skin, heavy or prolonged menstrual periods (menorrhagia), and spontaneous abortion.
Finally, Oropouche is capable of causing infection in the central nervous system, as observed in previous outbreaks, with evidence also raised in laboratory studies. Therefore, it is important to be aware of severe headaches. This symptom in particular becomes relevant since it can precede the development of aseptic or viral meningitis. Thus, in this case, symptoms include a stiff neck, dizziness, nausea, vomiting, lethargy, double vision (diplopia), and an involuntary and repetitive movement of the eyes (nystagmus), which can persist for up to two weeks.
Despite this long list of symptoms (some of which are quite serious), or pouches fever can be treated without any after-effects. In this sense, we emphasize the importance of diagnosis and medical follow-up.
Does this virus have great potential to spread?
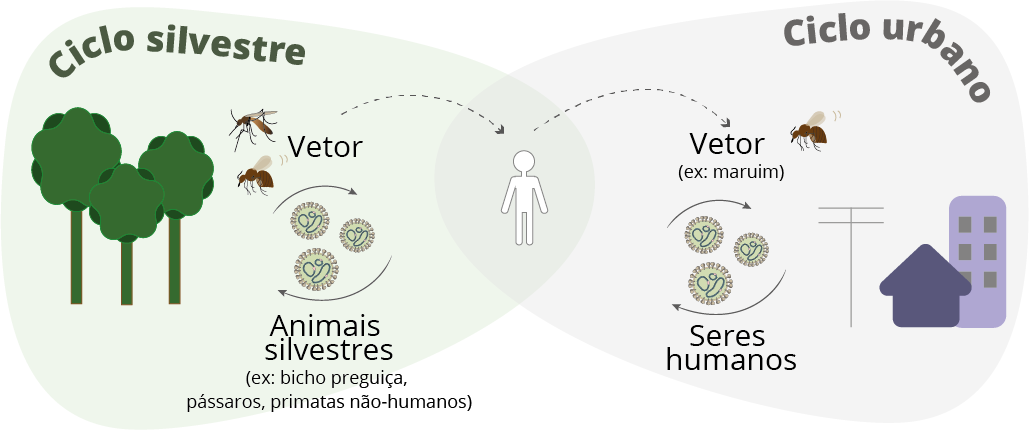
First, let’s look at the two transmission cycles of the virus, as shown in Figure 2. Oropouche circulates in forest regions (wild cycle) and can infect wild animals such as sloths, non-human primates, small rodents, and birds. The vectors of the virus, that is, those responsible for transmitting the disease, are mosquitoes, which are still little studied by science.
In addition, Oropouche also circulates in urban areas (urban cycle) in humans, transmitted by the bite of small hematophagous flies, also known as maruim or sand flies. The species Culicoides paraensis, found mainly in the northern region of Brazil, is indicated as the main vector (Figure 2). When humans enter forests, they can contract the virus and take it to urban areas, acting as a “bridge” between the two cycles (Figure 2).
Figure 2. The wild and urban cycles of the Oropouche virus.
Figure 3. Culicoides paraensis , the sandfly or sandfly. Image credits: Maria Luiza Felippe-Bauer, Instituto Oswaldo Cruz, Rio de Janeiro, RJ, Brazil.
It is always important to remember that severe changes in the environment are part of the increase in diseases like this!
As human interventions in forests and wildlife have intensified over the years, the chances of new outbreaks have also increased. Studies point to an increase in the number of Oropouche cases in regions impacted by fires and other activities that promote deforestation.
Now we have a second point: the vectors. Furthermore, regarding C. paraensis, it has already been demonstrated that more common mosquitoes, such as the species Culex quinquefasciatus (the famous and insolent mosquito), found in several regions of Brazil, the Americas, among other continents, are also a potential vector of the virus.
In other words, we need to be careful, don’t we?
After all, the diversity of vectors may favor the circulation of the virus beyond the Amazon region. Cases of Oropouche have already been identified in other locations, such as São Paulo, Bahia, Curitiba, and more recently in Rio de Janeiro, originating from travelers who had been to the North region.
Genome rearrangements and genetic variability
The universe of viruses, as well as their history, is intriguing! And we already know how important it is to study their submicroscopic structure. Researchers in Manaus have managed to identify a particularity in the genome of the Oropouche virus that is causing the current outbreak.
What would it be?
You see, after the COVID-19 pandemic, it became clear that we need genomic surveillance linked to epidemiological surveillance. To monitor variations in viral genomes that may favor its spread. What was observed in Oropouche samples from the current. The outbreak was a genetic variation in which there was a rearrangement of viral segments, a phenomenon known as “gene reassortment”. This phenomenon can occur between viruses with segmented genomes. In which two particles of the same species, but with some genetic differences, infect the same cell. In these cases, a rearrangement of the segments occurs at the time of production of new viruses. This results in the generation of hybrid viral descendants, with a unique combination of genetic characteristics (Figure 4).
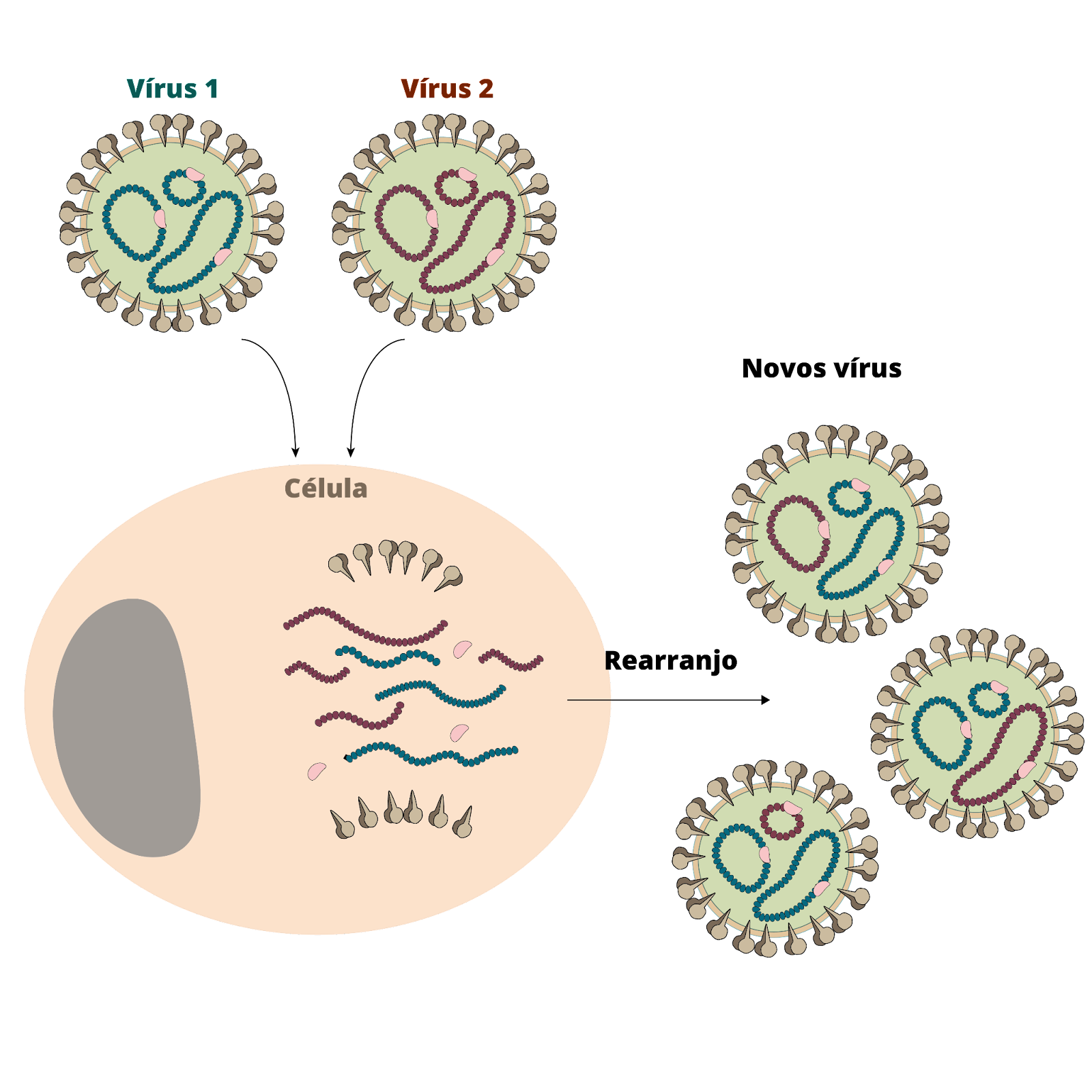
Figure 4. Genetic rearrangement, or reassortment.
It is important to know that this may have an impact on the emergence of new outbreaks.
Influenza A viruses, for example, are also segmented, and reassortment between two variants can occur, which confers genetic variability. This event is key to the emergence of new Influenza A viruses that cause major pandemics.
And what do we know about increased genetic variability in the context of viruses?
We know that this can bring some benefits to the virus. Including escaping the immune response, or even better adaptation to vectors. Which is also something to worry about and needs to be investigated!
But that subject will be left for our next text!
Therefore, let’s be alert to the emergence and reemergence of arboviruses, of which there are many. Have you ever heard of Oropouche fever?
To read More Informative Content Related to Science Subscribe to Us. Thank You!